|
We know that
everyone forgets things sometimes and that people become more forgetful as they
grow older. Even though a number of older persons who are normal occasionally
forget things and events, they are still able to do many of the activities that
they were able to do before. For example: cooking, reasoning, and planning
without assistance from others.
Serious
forgetfulness, mood swings and other behavioral changes are not a normal part of
ageing. They could be caused by different diseases like dementia and depression
or other medical conditions. Poor diet, malfunctioning thyroid, lack of sleep or
too many medicines are other factors that could influence it. Feelings of
loneliness and boredom or depression can also cause forgetfulness. These
conditions can often be treated and medical advice should be sought
When someone
has dementia, they may forget the names of not only strangers but also family
members. They may forget whether they have eaten lunch. They may repeat the same
question again and again and not be aware of the fact that they are doing it.
They may need help with even simple daily activities, such as dressing, eating
or going to the toilet. This is not normal forgetting.
Dementia can
happen to anybody, but it is more common after the age of 65 years. About 3% of
persons, who are over 65 years of age, suffer dementia. The chances of having
dementia increase with the age of the person. However, people in their 40s and
50s can also have dementia.
What is
dementia?
Dementia is the
general term for a gradual progressive decline in a person’s memory and other
mental abilities and ability to do things effectively. Dementia itself is not a
disease. It is a condition (sometimes called a syndrome) that can be caused by
many diseases. Dementia is disease related-not just a memory problem. Dementia
refers to impaired memory as well as changes to at least one of the following
areas:
-
Language
-
Reason
-
Perception
-
Judgment
-
Abstraction
-
Organization
-
Attention
In medical
terms, these impairments are said to be global. This means that it affects many
abilities of the brain.
Memory:
Memory involves learning and remembering new information and past experiences.
In the beginning stage of dementia, memory problems affect recent memory. The
person understands what you say at the time and responds appropriately but may
not recall (be able to remember) the incident a short time later. Towards the
middle stage of dementia, both recent (memory of events that have occurred
recently) and long term (memory of events that have occurred in the remote past)
memory are declining. In the late stage of dementia, the person is no longer
aware of names, has trouble recognizing familiar people, and cannot recognize or
use familiar objects.
Language:
Language involves the ability to use both voice and written symbols to
communicate thoughts and feelings. The first language problems usually involve
word finding. The person may not be able to
remember the names of people who are known or find the right words in
conversation. This may lead to embarrassment and frustration. Eventually the
person may withdraw from socializing. As the disease progresses, the person may
find it hard to express ideas or clearly communicate what he or she wants
to say. By the late stages of the disease, the ability to speak or understand
language declines.
Sensory
perception: We use our sensory abilities (Five senses of seeing, hearing,
smelling, taste and touch) to become aware of our environment in dementia, the
brain is less able to interpret this information from the five sense organs.
This is what causes perception problems such as difficulty
with space perception, identifying objects, perceiving distances and
understanding words and directions. Even when the person can see and hear
clearly, the object may not be understood accurately. The following may result
in misunderstanding of what is happening around, suspicion, illusion
(misidentification of objects or people) and delusions (false beliefs).
Organization: In order to perform tasks and activities, our ideas and
movements must be coordinated. Most of our actions are over-learned. This means
that we do things easily without realizing our brain is directing our body to
move. The person with dementia however begins to have trouble figuring out how
to do things and doing the tasks in a step-wise manner. By the end of the
disease, the person will lose the ability to do all purposeful activities.
Abstraction:
To think abstractly we use images and thoughts to consider possibilities of a
situation. The ability to reason is basic to a person’s functioning
independently and safely. We use abstract thinking (symbols, hypothetical
situations, etc) to consider the relationship between different ideas and to
predict outcomes.
As the ability
to reason becomes more concrete, the person
-
Loses the
ability to solve problems and make judgments
-
Does not think
ahead or consider the whole picture
-
No longer sees
the cause and the effect
- Bases choices on superficial
visual information (what he sees without understanding the meaning of the
context)
-
Takes one step
at a time using trial and error approach
-
Needs visual
cues to focus on things that can be seen
Attention/
concentration: Attention can include the ability to start, maintain and stop
a task. As the dementing illness progresses, the attention span shortens. The
person becomes less and less able to focus attention or move from one step to
another. In the beginning stage, many persons appear to be lazy or depressed,
but they are simply unable to focus their attention and start a task. When
someone helps them start, they may do well. By the middle stage, the person may
not be able to shift from one action to another. Successful activities include
those with repetitive one-or two-step actions such as: folding, sweeping,
dusting, wiping and stacking.
Near the late
stage, the person will repeat the same motion over and over. A man with dementia
may shave the same spot until reminded and directed to move to another spot.
Judgment:Judgment
is the capacity to use information and make the right choices. The person’s own
awareness of his or her loss of abilities vary greatly from individual to
individual and changes as the illness progresses. Some individuals may become
hesitant use more caution than before and begin to rely more on others. Other
individuals seem to lose inhibitions and the sense of caution, become impulsive
and act without considering the consequences. When judgment is impaired, safety
becomes a main issue. The person’s faulty reasoning may mean that he or she is
unsafe to be alone. By moderate to sever dementia, abstract thought is too
impaired to allow the person to identify problems and hazards. The caregiver
must take increasing responsibility as the person’s judgment becomes impaired.
A person does
not need to have all of these difficulties to be diagnosed as dementia. The
definition refers to a gradual and progressive decline in memory and at least
ONE of these areas for the condition to be diagnosed as dementia.
These facts
about dementia refer to a person’s mental abilities but dementia does not affect
only a person’s thinking abilities. It also affects their abilities to do
things. They may have difficulties in shopping, driving, managing finances; as
well as difficulties in getting dressed, bathing, and using the bathroom
Dementia knows
no social, economic, ethnic or geographical boundaries. Every person with
dementia is different How the illness affects a person depends on which areas of
the brain are most damaged. Even if the person does not have difficulties in all
these areas, it will eventually be affected and will gradually develop over time.
The course and severity of these effects will vary from person to person. The
level of difficulty the person has in each of these areas may vary across the
area. Similarly, the rate at which the disease progresses varies in each person.
Even being tired or the presence of other illnesses can increase the problem.
Although each
person will experience dementia in their own way, eventually those affected are
unable to care for themselves and need help with all aspects of daily life.
What is the
course of dementia?
Dementia is a
progressive illness. From the start of the illness till its end, it may take
about 10-15 years. This depends on individual progression of the illness. People
with dementia differ in the patterns of problems they experience and in the
speed with which their abilities deteriorate. Their abilities may change from
day to day, or even within the same day. What is certain is that the person’s
abilities will deteriorate - sometimes rapidly over a few months; in other
cases, more slowly, over a number of years. Depending on the cause, reversible
dementias may recover or be cured.
Features of
dementia are commonly classified into three stages or phases. It is important to
remember that not all of these features will be present in every person, nor
will every person go through every stage.
Early or
mild dementia: Often one realizes the symptoms of the disease in this phase
after the person has passed the particular stage. During the disease phase, it
may be missed, or explained as old age or overwork. The start of dementia is
very gradual, and it is often impossible to identify the exact time it begins. A
person in the early stage of dementia will be able
to do most everyday activity without help - though mistakes may happen. During
the early phase of dementia, the person may:
- Appear more apathetic, with
less sparkle.
- Lose interest in hobbies or
activities.
- Be unwilling to try new
things.
- Be unable to adapt to
change.
- Show poor judgment and make
poor decisions.
- Be slower to grasp complex
ideas and take longer with routine jobs.
- Blame others for ‘stealing’
lost items.
- Become more self-centred and
less concerned with others and their feelings.
- Become more forgetful of
details of recent events.
- Be more likely to repeat
themselves or lose the thread of their conversation.
- Be more irritable or upset
if they fail at something.
- Have difficulty with complex
tasks that they used to do like handling money, find their way around the
town, go shopping, etc
Middle or
Moderate dementia: During the ‘moderate’ phase, the person’s problems are
more visible and affect the person more. The middle stage is generally very
long. In this stage, the person gradually loses the ability to do tasks - even
simple tasks without help, and complicated tasks will be beyond his or her
abilities. They may:
Be very
forgetful of recent events. Memory for the distant past seems better, but
some details may be forgotten or confused.
- Be confused regarding time
and place.
- Become lost if away from
familiar surroundings.
- Forget names of family or
friends, or confuse one family member with another.
- Forget having kept utensils
on the stove. May leave gas unlit.
- Wander around streets,
perhaps at night, sometimes becoming lost.
- Behave inappropriately - for
example, going outdoors in their nightwear.
- See or hear things that are
not there.
- Become very repetitive.
- Be neglectful of hygiene or
eating.
- Become angry, upset or
distressed through frustration.
Late or
Severe dementia: During this later stage of dementia, the person is severely
affected and needs total care. At this stage, the person may:
- Be unable to remember - for
even a few minutes - that they have had, for example, a meal.
- Lose their ability to
understand or use speech.
- Be incontinent.
- Show no recognition of
friends and family.
- Need help with eating,
washing, and bathing, using the toilet or dressing.
- Fail to recognize everyday
objects.
- Be disturbed at night.
- Be restless, perhaps looking
for a long dead relative.
- Be aggressive, especially
when feeling threatened or closed in.
- Have difficulty walking,
eventually perhaps becoming confined to a wheelchair.
- Have uncontrolled movements.
Immobility
(Inability to move around) will become permanent and, in the final weeks or
months, the person will be bedridden. Dementia is a progressive illness. Death
is usually from a complication of a physical illness.
What causes
dementia?
Dementia can be
caused by various diseases that in a gradual and progressive manner, cause
damage to the parts of the brain involved with the thinking processes. Dementia
is not caused by:
-
Under use or
overuse of the brain
-
Other mental
illnesses
-
Sexually
transmitted diseases
-
Infection
-
Aluminium or
other metals
Most cases are
caused by Alzheimer’s diseases or vascular dementia. All of the types of
dementia cause similar symptoms, but some features may point to a particular
cause. Research is ongoing and factors which might be important in determining
why certain people develop dementia are being looked into. Factors such as the
environment, diet, drugs, education levels and genetics are all being
researched.
Alzheimer’s
disease (AD): Scientists still do not fully understand what causes Alzheimer’s
disease. Alzheimer’s disease destroys brain cells and nerves blocking the
transmitters, which carry messages in the brain, particularly those responsible
for storing memories. Alzheimer’s disease was first described by Alois Alzheimer
in 1906.
Scientists
believe that whatever causes Alzheimer’s disease begins to damage the brain
years before symptoms appear. When symptoms emerge, nerve cells that process,
store and retrieve information have already begun to degenerate and die. The
brain reduces in size as gaps develop in the different parts of the brain such
as temporal lobe and hippocampus, which are responsible for storing and
retrieving (remembering) new information. This in turn affects people’s ability
to remember, speak, think and make decisions. The production of certain
chemicals in the brain, such as acetylcholine is also affected. It is not known
what causes nerve cells to die but there are characteristic appearances of the
brain after death. In particular, ‘tangles’ and ‘plaques’ made from protein
fragments are observed under the microscope in damaged areas of brain. This
confirms the diagnosis of Alzheimer’s disease.
Amyloid plaques
are clumps of protein that accumulate outside the brain’s nerve cells. Tangles
are twisted strands of another protein that form inside cells. Scientists
do not yet know whether plaques or tangles cause Alzheimer’s or are caused by
some other processes.
Late-onset
Alzheimer’s, which chiefly affects individuals over age 65, is the more common
form of the illness that is most often associated with the term “Alzheimer’s
disease.” The greatest known risk factors for late-onset Alzheimer’s are
increasing age. Recent research seems to show that like other diseases, there
may also be a genetic factor in dementias. However, this does not mean that
someone whose parent had Alzheimer’s will automatically develop the disease.
Vascular
dementia accounts for about 30-35% of all cases of dementia. Vascular disease
occurs where blood vessels are damaged and the supply of oxygen is at risk. The
most common type of vascular dementia is multi-infarct dementia (MID) where the
brain has been damaged by repeated small strokes.
When any part
of the body is deprived of blood, which carries oxygen and nutrients, it dies
and this is called an infarct. When this happens in the brain it is called a
stroke. The mini strokes that cause vascular dementia are often so slight that
they cause no immediate symptoms, or they may cause some temporary confusion.
However, each stroke destroys a small area of cells in the brain by cutting off
its blood supply and the cumulative effect of a number of mini strokes is often
sufficient to cause vascular dementia.
Depending on
where the stroke occurs in the brain, different functions of the brain will be
affected. It can cause problems with language, memory, recognition of objects
and coordination of complex tasks. Strokes in certain areas of the brain can
also cause changes in the person’s mood and personality.
Vascular
dementia can be caused by a number of conditions including high blood pressure
(hypertension), irregular heart rhythms (arrhythmias), diabetes and diseases,
which cause damage to the arteries in the brain. Indeed, any condition, which
causes the circulation to the brain to be impaired or damaged, carries a risk
for strokes to occur.
Vascular
dementia is similar to AD in that it results in progressive deterioration of the
higher functions of the brain. One major difference with vascular dementia is
that these changes will generally occur in a stepwise pattern due to the sudden
occurrence of strokes.
The person will
usually deteriorate at the point that they have a stroke, but they may improve
or remain stable for a while before the next stroke occurs, when they will again
deteriorate. It is often difficult to decide with certainty whether a
person has Alzheimer’s disease or vascular dementia and often a patient will
have both types of dementia.
Other causes
are:
1. Fronto
Temporal Dementia (FTD): Fronto-temporal dementia refers to a group of
related dementias which begin in the brain’s frontal lobe, temporal lobe; or
both lobes together. The cluster of symptoms will vary according to the degree
of involvement of the frontal and temporal lobes and which side of the brain is
affected. It typically occurs earlier than Alzheimer’s disease and may have
personality or language changes as early symptoms.
2. Alcohol
related dementia: Prolonged use of alcohol, particularly if associated with
a diet deficient in thiamine (vitamin B1), can lead to irreversible brain
damage. This dementia is preventable. The most vulnerable parts of the brain are
those used for memory and for planning, organizing and judgment social skills
and balance. If drinking stops, there may be some improvement Taking thiamine
appears to help prevent and improve the condition, once off alcohol.
3. AIDS
related dementia: HIV, the virus which leads to AIDS, can be a cause of
dementia. The virus has been found in the brain of people with HIV as early as
two days after initial infection. This condition is usually referred to as AIDS
dementia complex (ADC)
4.
Parkinson’s disease: Parkinson’s disease is a progressive disorder of the
central nervous system, characterized by tremors, stiffness in limbs and joints,
speech impediments and difficulty in initiating physical movements. Late in the
course of the disease, some people may develop dementia.
Other causes
are Huntington’s disease and Lewy body dementia
Treatable or
Reversible causes of dementia
There are a
number of conditions, which have symptoms of dementia. By treating these
conditions, the symptoms will often disappear. These include:
It is essential
that a medical diagnosis is obtained, usually by doing a brain scan, at an early
stage, when symptoms first appear, to ensure that a person who has a treatable
condition is diagnosed and treated correctly.
How can
medication help?
There is an
immense amount of research into new drug treatments for Alzheimer’s disease and
the other dementias. While there are no drugs that can cure Alzheimer’s disease
there are drugs, which can help remove some of the symptoms of dementia disease
and improve their quality of life by stopping the progression of disease.
Three drugs are
commonly prescribed-Donepezil, Rivastigmine and Memantine. All of these drugs
are designed to prevent the breakdown of acetylcholine, a chemical messenger in
the brain that is important for memory and other thinking skills. The drugs work
to keep levels of the chemical messenger high, even while the cells that produce
the messenger continue to become damaged or die. About half of the people who
take cholinesterase inhibitors experience a modest improvement in cognitive
symptoms. .
On the MMSE, a
clinical measure of the patients functioning, those who do not take medication,
show a significant deterioration (may drop 3-4 points) whereas those on
medication may remain at the same level or have minimal deterioration in
comparison.
However, these
drugs do nothing to stop the death of the nerve cells in the long run, so they
will not bring a permanent cure. Side effects of these drugs include diarrhoea,
nausea, insomnia, fatigue and loss of appetite, which are reduced by gradually
increasing the medication.
Memantine is a
drug for treatment of moderate to severe Alzheimer’s disease. It appears to work
by regulating the activity of glutamate, one of the brain’s specialized
messenger chemicals involved in information processing, storage and retrieval.
Glutamate plays an essential role in learning and memory. Memantine may be
combined with other medicines for better effect It acts by halting further cell
damage.
Other kinds of
medicines are sometimes useful for controlling some of the symptoms of
Alzheimer’s disease, such as sleeplessness, agitation, aggression, hearing
voices, false beliefs etc. These medicines are commonly used to treat mental
illnesses.
For vascular
dementias, Aspirin is widely used to lessen the risk of further strokes by
preventing clots from forming in small blood vessels. There are also drugs
available to control high blood pressure, diabetes and high cholesterol levels.
Drugs to control depression and relieve restlessness and help the person with
vascular dementia to sleep better can also be prescribed.
SESSION 2
One method of
reducing the confusion experienced by the person with dementia is to establish a
routine. A routine would involve certain tasks or activities that the person
could do to keep them occupied as well as provide them with a sense of security
and familiarity. It also reduces the burden experienced by the caregivers.
However as dementia affects the abilities of a person, the caregiver needs to be
able to identify the activities that fit the remaining abilities of the affected
person.
Completing an
activity successfully involves three basic components:
Purpose:
Purpose refers to knowing and keeping an end goal or purpose in mind when doing
the task. It helps us to make a plan on how to do a task as well as to carry out
the task successfully.
Order: Order
refers to the sequence of steps one needs to have to finish the task. Sometimes
there is only one way of doing it, sometimes there are different ways of doing a
task. The main thing to remember is that whichever correct method one uses,
there was an order - it was not random.
Use: Use refers
to being able to use the necessary tools or objects appropriately. This involves
not only how to use but also when to use it.
In Dementia,
the person loses their capacity for these elements-purpose, order and use. A
caregiver needs to remember this when they give them tasks to do. Are they able
to remember the purpose of the task? Are they able to do the steps in the right
order to finish the task? Are they able to make use of the things required for
the task?
The Allen
levels of Performance is an approach used by Occupational Therapists to estimate
the ability of a person with dementia. The caregiver can learn at which level
their family member is and what needs to be done for them at this stage.
In this
approach, the highest functional level is Level 6, where there is normal
thinking. The lowest level is Level 1 , which is the end of the disease process.
These levels form a continuum of how the person’s abilities are affected. This
can be related to the memory stages covered in the first session. Level 5
would approximate Early Dementia and Levels 4 and 3 would approximate
Middle and levels 2 and 1, are Late stages.
LEVEL 6:
NORMAL THINKING
CAN
PROCESS COMPLEX INFORMATION CAN ANTICIPATE, CONSIDER AND AVOID CAN READ/
WRITE/ CALCULATE AND PLAN -
CAN:
MANAGE FINANCES, LIVE ALONE, PREPARE MEALS, DRIVE, BE IN COMPETITIVE EMPLOYMENT
Level 6
consists of the normal expected abilities
Level 5
is an early stage of the dementia. The person at this level may appear to be
functioning quite normally in many situations and may show signs of the problem
only when under stress. Persons vary in the amount of insight they have about
having the disease. Some seem to understand there is a problem and are able to
talk about it. Some become depressed and others might not be aware or might deny
awareness
LEVEL 5: FIRST
SIGNS (EARLY OR MILD DEMENTIA)
-
RELATIVELY ABLE
AND INDEPENDENT
-
PROBLEMS WITH
SHORT TERM MEMORY
-
PROBLEMS LOSING
TRACK IN COMPLICATED TASKS
-
PROBLEMS WITH
PLANNING, PROBLEM SOLVING AND JUDGMENT
-
SHOULD BE ABLE
TO MANAGE MOST CONCRETE TASKS
-
MAY BEHAVE
IMPULSIVELY OR HESITANTLY
The person is
able to function independently in most areas of life. They will experience
difficulties with complex tasks - tasks that require many steps and abstract
thinking. They may have to quit their jobs earlier than they had expected to
because they can no longer handle the difficulties of the job.
If the
equipment is selected and set out for the person, thereby not relying on the
person’s planning or judgment, they would be able to do a task easily. The
person is able to remember quite well the purpose of the task, the order and the
use of the objects given. .
Level 4:
In this level, which approximates the middle stage of dementia, the person looks
for cues in the environment as to what to do. Thinking appears to be guided by
visual information and verbal direction from others. They may lose track of
time, may not know what to do and may become anxious. Complex activities need to
be done by others. Performance of daily activities like bathing and changing is
inconsistent-they may resist. Misinterpretations are common as they are unable
to consider alternative explanations and ideas. They need daily supervision and
assistance.
LEVEL 4:
SIGNIFICANT IMPAIRMENT (MIDDLE/ MODERATE DEMENTIA)
-
LIMITED
ATTENTION & EASILY DISTRACTED-REACTS TO PRESSURE, NO ABSTRACT THOUGHT
- NEEDS SIMPLE AND FAMILIAR
TASKS WITH FEW STEPS
- KNOW THERE’S A GOAL, BUT
NEEDS REMINDERS
-
CLEAR TROUBLE
WITH MEMORY, LANGUAGE, ORGANIZATION, PERCEPTION AND ATTENTION
- PERFORMANCE QUALITY IS POOR
- NEEDS HELP ORGANIZING TASKS
- NEEDS SHORT, CONCRETE
DIRECTIONS-VISUAL CUES
It is possible
that a person with dementia may not have reached this stage and may be in
between this and the previous stage. They may still be relatively independent in
that they can take care of their needs unless some physical problem is present.
They will make more errors and will need more prompting and reminding.
Depending on
their awareness of and sensitivity to their own condition, persons at this stage
may become more withdrawn unless encouraged to remain a part of things. They may
show frustration at their own inabilities and may become more emotionally
difficult.
They will still
have a sense of purpose, order and use although since judgment is more impaired,
safety is an issue with use of objects. Written information may become less
useful though verbal information should still be effective.
Level 3:
Level 3 is also seen in persons in the middle or moderate dementia. It is
observed more towards the latter part of the middle stage, whereas level 2 is
seen more in the beginning stages of middle dementia.
At this level,
they confuse the past and present, are not aware of the goal of tasks and do not
understand the activities that are going on around them. They focus on objects
and like to handle and move things without a clear purpose in mind. The
caregiver finds it easier and faster to do basic activities for them rather than
try to make them understand or participate. They need constant supervision as
they move around with no awareness of dangers. Although speech is limited they
usually enjoy being with other people.
LEVEL 3:
GENERAL CONFUSION (MIDDLE/ MODERATE DEMENTIA)
-
ALL THINKING
POWERS SERIOUSLY AFFECTED
-
VERY CONFUSED;
HARD TO UNDERSTAND WHAT’S HAPPENING OR
WANTED OF THEM
-
NO PURPOSE;
ORDER WITH HELP
-
NEEDS HELP
STARTING AND STAYING WITH ALL TASKS
-
VERY
CONCRETE-VISUAL AND TACTILE CUES
-
STEP BY STEP
HELP
-
VERY EASILY
DISTRACTED, FRUSTRATED, UPSET, CONFUSED. DO NOT RUSH OR
PRESSURE-REASSURE
It is possible
a person with dementia may not have reached this stage and may be at a stage
between Level 4 and 3. The person would be vague about the purpose and may not
feel there is any. They may be able to do 2-3 steps of the task on their own,
but need help in starting and with steps throughout a task as a result. They
need visual and tactile information and their thinking may be impaired. They may
not remember who the caregiver is. As they still can do many things, it would be
useful to allow them to do however with supervision
Level 2:
Level 2 is the late stage or severe dementia. A person at this stage becomes
totally dependent on others. The person’s physical condition, including balance
and walking declines. The person loses the ability to use or handle objects but
may still grasp and hold on to things. They are most aware of touch and things
that come in direct contact with them. Movements and sounds also draw
their attention. They may resist care at times because they are confused or
frightened. They require almost complete care and are no longer capable of doing
much for themselves except to cooperate passively.
LEVEL 2:
MINIMAL ABILITIES (LATE/ SEVERE DEMENTIA)
-
POWERS OF
THINKING VIRTUALLY GONE
-
DO NOT HAVE
PURPOSE AND ORDER
-
MAY OR MAY NOT
RELATE TO OBJECTS
-
NEED TOTAL CARE
Level 1:
Level 1 is also a late/ severe dementia, and is seen more towards the end of the
disease stage. These individuals lose awareness of their surroundings. Most
movements are reflex movements such as towards light or pain. The person may
focus on objects that move in front of them. They lose the ability to walk or
communicate and require total care.
LEVEL 1:
BED-RIDDEN (LATE/ SEVERE DEMENTIA)
The caregiver
should attempt a rough estimation of which level their family member is at. Even
if the estimate is incorrect, perhaps too high or too low, that is fine. As the
family member does the task, the caregiver will be able to understand better
their level and adjust their estimation. It is important to remember that
sometimes a person’s level will vary from day to day depending on a number of
factors. If the person is ill or has not slept well or has recently been very
upset, then his performance ability may be lower than usual. There are also some
tasks which are very familiar and which they may have practiced doing many
times. They should still be able to do these tasks for a longer time than other
tasks. It would help to think of examples such as bathing, dressing, eating etc.
to base one’s assessment on to get a sense of which level the family member is
functioning at now.
Aside of being
aware of the abilities of the person and the components of a task, a caregiver
should also consider the dimensions of a task when fitting it for their family
member. The dimensions of tasks involve:
Size: Size
refers to the number of steps that are involved in a task. For example, in
cooking, we need to select the ingredients, cut the vegetables, etc.
Complexity:
Complexity refers to the amount of abstract thinking involved in completing the
task such as the purpose of the task, whether the things required are absent and
the person has to find them.
Space/distance:
Space or distance refers to whether the task takes place in front of the person
or in the same room - does the person have to move out of the room to complete
the task?
Time: Time is
similar to steps in that it has to do with the amount of time expected for the
person to repeat the task and to stay with repeating the task.
Skills: Skills
refer to whether the person has the basic skills required to do the job. Some
things may be simple for us but may be difficult for others.
In almost
all the activities that a caregiver can think of, there is a process
of ongoing assessment that is necessary. In this process, the caregiver
uses what they know about the person to adjust the kind of task to be
given, the way in which the task is set up and the help they would give
to get and keep the person going in the task. At the same time, a caregiver
has to use their observation of how the person reacts to a particular
activity on a given day to readjust their estimate of the person’s
overall ability to perform tasks.
Caregivers
will need to choose tasks that are the right size and complexity for
the person at a given moment. This could involve avoiding tasks that
require planning, simplifying tasks, allowing more time, limit choices,
handing objects, setting everything up in order of use, etc
They will
need to decide how much help they will need to do the task. Each person
will require different kinds and amounts of help to get started with
and keep going in their parts of the task. This can be any form of communication
such as written, verbal or visual directions, demonstrations, instructions,
reminders of steps and purpose, cues, guiding touch, examples of finished
product, positive tone, humour, relax expectations, etc
As the illness
progresses, the caregiver will need to modify the activities and approach in
caring for them. What works one day, may not work another day. The caregiver
needs to remember this is a skill that he is developing, and needs to work at
it. It will not be easy the first few times, but gradually with practice and
perseverance, one will have some success. Even if the caregiver does not
succeed, they will learn what works and what does not. The caregiver can use
this knowledge in their future efforts.
SESSION 3
COMMUNICATION AND DECISION
MAKING
Care giving
is often difficult and frustrating. Along with day to day care giving
tasks, there are other decisions that need to be made, these range from
everyday concerns such as how to communicate to your family member,
how much help to provide in daily activities like bathing or dressing
and long term decisions such as how to provide for them financially.
There
are some basic points the caregivers need to remember when communicating
with a person with dementia.
When speaking
to the person, first make
sure that you have their attention.
Do not assume they are paying attention to you. There are many things
around them that could distract them - like an untidy room, a bright
light too much noise, etc. Give them some time to recognize you are
there and to focus on you before you start talking to them.
As their
perceptual abilities diminish, you can avoid
approaching them from the side or the back -
this will surprise them and they may get confused. If they have any
eyesight or hearing difficulties, make sure they have spectacles or
hearing aids.
When speaking
to them, it helps if you speak loud enough for them to hear you. But
you must not sound angry! Use
simple words, short sentences as
well. As the disease progresses, rely less on language and more on visual and tactile cues.
These
guidelines are broad estimations - they are not specific. Be flexible
in one’s approach; try different kinds of tasks and activities, even
new ones. See what best suits the person.
Apart
from communicating effectively and caring for the family member, the
caregiver also has other responsibilities such as a job or household
activities. And for some caregivers, they may have to do both, job and
household chores. There are also other family members to provide for
or care for as well.
Prior
to the person’s illness, the person could contribute towards these
responsibilities. Some caregivers may not have been working before their
illness. Some even though they may have been working, may not have had
as much pressure on them as they do now. In many ways, the person was
able to help whether for simple things around the house or to discuss
problems. But most of caregivers have to manage alone.
For some
people, major decision-making is a new experience, an added role and
responsibility. Sometimes other family members can provide support in making
decisions but they may have different opinions about what to do, lack all the
details or live too far away to provide practical help.
 |
|
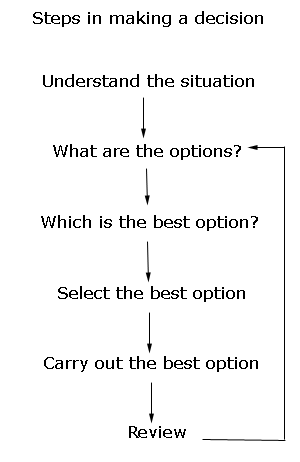
The first
thing to do when we need to make a decision is to assess or understand
the situation well. Suppose the caregiver and the person lives alone.
Upon awakening from a nap, the caregiver discovers the person has wandered
away from home again. Now upon finding and bring them back, what is
the decision that the caregiver needs to make in this situation? The
caregiver needs to decide what to do about the person’s wandering.
In this first
step, the caregiver understands the situation by assessing and determining the
required goal. In the example, the goal is to prevent the family member from
wandering and getting lost. After understanding the situation and determining
the goal, the caregiver has to identify options to prevent or reduce the
wandering.
Upon
identifying the options available, the caregiver has to decide which of them to
choose. The third step is then to evaluate each of these options and determine
to the best of one’s ability, the option that will lead to the goal. Your
previous experience as a caregiver as well as your knowledge obtained from the
treating team may help you to decide. The caregiver weighs the advantages and
disadvantages of each of these options before deciding which one would be the
most likely to succeed. The caregiver needs to keep in mind the person’s
abilities-their abstraction, ability to reason, judgment, etc.
Upon
identifying the best option, the caregiver must implement the option. The
caregiver keeps in mind that the person’s abilities may vary from day to day or
even within a day, and other factor such as being tired, over-stimulated etc may
influence the person. Thus the caregiver should not give up when on the first
attempt they do not succeed. They may need to try the option a few times before
deciding whether it is successful or unsuccessful.
|
If upon attempting
a few times, the caregiver does not find the option to be
successful, the caregiver needs to be flexible. Depending on the condition of
the person, the situation may change and one may need to revise the decision.
The caregiver may need to further understand the situation and generate other
alternatives.
Initially
the caregiver may find it difficult to pause and think of these steps.
But as they get used to it, it will be easier. Sometimes just
thinking about the different available options will make it easier to
decide. This process of making decisions is most useful when the caregiver
has complex and difficult decisions to make as well as for everyday
management of the person.
There
are also a number of long-term decisions that a caregiver will need
to make, such as: if they are the only caregivers, then should anything
happen to them, who would care for their family member? Or if the family
member has banking or legal responsibilities, what do they need to do?
There are a number of such decisions that a caregiver will need to think
about.
The caregiver
may perhaps be concerned about what the family member will think or
feel if they take over their finances or how they may feel when the
caregiver tells them how to do something. As the disease progresses,
the person’s self-esteem reduces and so the caregiver should not be
as worried about how they may feel.
|
